Definition of Pain
“Pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage”
-IASP, 1979
Postoperative Pain in Pediatrics
- Pediatric patients often receive inadequate pain management.
- Unrelieved pain has potentially dire consequences for our patients.
- Fear of pain is a source for great distress in children and adolescents e.g. what will happen next? What is going on? Why do I feel this way?
- Increased attention to pain relief improves satisfaction with medical treatment.
- There are many effective treatments for pediatric pain. Using non pharmacological treatments along with medications substantially improve patients outcomes.
- Organizational culture and pain team approaches are important to improving pain management and updating believes and attitudes of healthcare providers.
Common Causes of Pain in Pediatrics
All Children
- Headache
- Oral/dental pain
- Abdominal pain
- Musculoskeletal pain
- Limb pain
- Back pain
Hospitalized Children
- Cancer pain
- Abdominal pain
- Back pain
- Postoperative pain
Prevalence of Moderate-Severe Pain after Surgical Procedures in Hospitalized Children
| Surgical Specialty | Prevalence Mod-Severe Pain (%) |
|---|---|
| General surgery | 65 |
| Plastic surgery | 47 |
| Neurosurgery | 42 |
| ENT | 38 |
| Urology | 36 |
| Orthopedics | 35 |
Types of Pain
Nociceptive Pain
Caused by activity in neural pathways in response to potentially tissue-damaging stimuli.
- Postoperative pain
- Arthritis
- Mechanical low back pain
- Pain from injuries
- Sickle cell crisis
- Pancreatitis
Mixed Type
Caused by a combination of both primary injury and secondary effects.
Neuropathic Pain
Initiated or caused by primary lesion or dysfunction in the nervous system.
- Postherpetic neuralgia
- Neuropathic low back pain
- Distal polyneuropathy (e.g., diabetic, HIV)
- CRPS
- Trigeminal neuralgia
- Central post-stroke pain
Learn About Scoliosis
Image
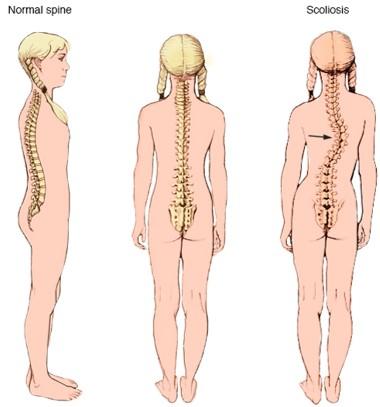
- Most common spinal deformity worldwide
- Causes curvature of the spine
- Spine sometimes looks more like the letter “S” or “C” than the letter “I”
- Spine can be rotated or twisted
- Pulls ribs to form multidimensional curve
- Peak prevalence: adolescents 10-18 years of age
- Can occur in younger children
- More likely to progress in girls
Etiology
Image
- Affects as many as 3 in 100 Americans
- Origin of idiopathic scoliosis remain unknown
- Research has shown it has a genetic component
- Continued research needed to determine specific genes and genetic markers
- Frequently detected in school screening
Signs and Symptoms
Signs and Symptoms of Idiopathic Scoliosis
- Difference in shoulder height
- Head is not centered with the rest of the body
- Difference in hip height or position
- Difference in shoulder blade height or position
- Tilted pelvis
- A difference in the way the arms hang beside body – when standing straight
- The sides of the back differ in height – when bending forward
- Clothing does not hang straight
- Mild or moderate scoliosis is not painful
- Mild idiopathic scoliosis does not cause any symptoms
- Parents/children may be concerned about cosmetic appearance of back
- 39% of patients with scoliosis severe enough to require surgery have mod-severe pain preoperatively but are not usually taking analgesics (Sieberg CB et al)
Adams Forward Bend Test
Image
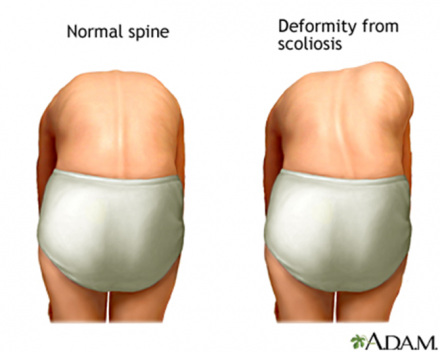
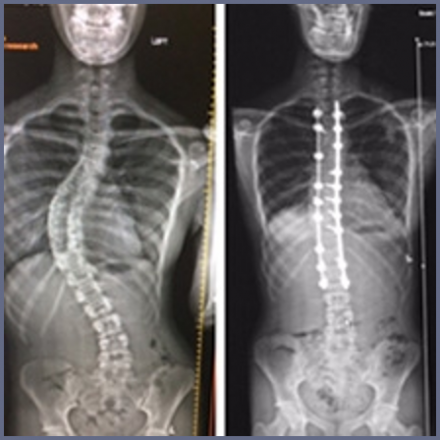
Courtney's Xray
- Thoracic curve 21
- Risser 2 (skeletal growth not complete)
Image
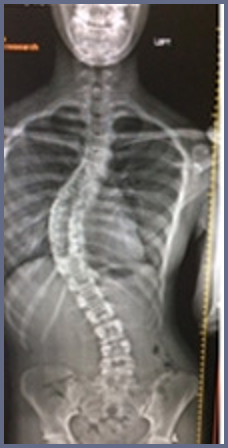
http://www.chop.edu/stories/scoliosis-courtney-s-story
Non Surgical Treatment: Back Brace
Image
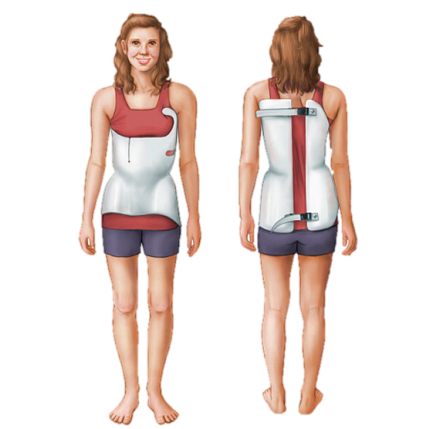
Courtney's Back Brace
Courtney talks about her treatment with her back brace.
Surgical Intervention: Spinal Fusion
Another treatment option is surgical intervention to fuse the spine.
Image
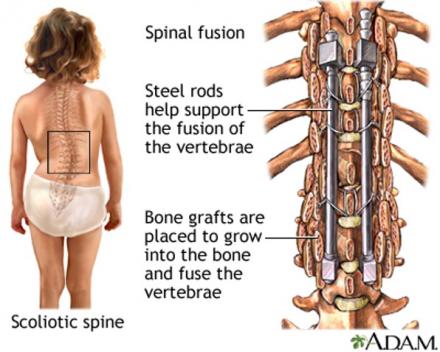
Spinal Fusion Pain
- One of the most invasive surgeries in adolescents
- Extensive tissue and bone trauma
- Involves severe post operative pain
- >7 on a scale of 0-10
- About half of all patients suffer from prolonged postoperative pain at the surgical site
Image
Bowel Medications While on Opioids
- Stool softener – Miralax, dulcolax
- Motility agent – Senna, bisacodyl (also available as suppository)
- Stomach protection
- H2 blocker (e.g cimetidine or ranitidine)
- Proton pump inhibitor (e.g. esomeprazole)
Instructions for Parents and Children
- Target 1-2 soft stool per day
- If stool is hard, increase stool softeners
- If frequency is less than 1 per day, increase motility agent

