Electronic Health Record (EHR)
Vital Signs, General Survey
- Vital Signs(VS): TEMP: 98.2; PULSE: 95; BP: 121/78; RESP: 16.
- General Survey (GS): No apparent distress, but quiet, sometimes frowning. Patient is well groomed. Patient ambulates well; no abnormal bodily movements.
- Head and Neck (HN): No pain to palpation of orbits, sinuses. No obvious head and neck trauma now or previously. No obvious abnormal facial movements.
Head and Neck Examination
HN
No asymmetry, no swelling, no obvious trauma. Piercings in R & L earlobes, L nares, no inflammation.
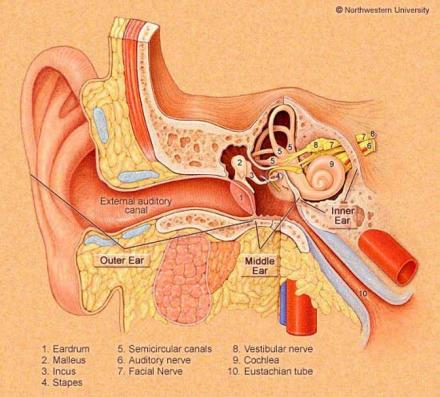
EAR
External Ear
External ear is slightly painful, as is tragus. No obvious trauma, inflammation, swelling, skin appearance normal.
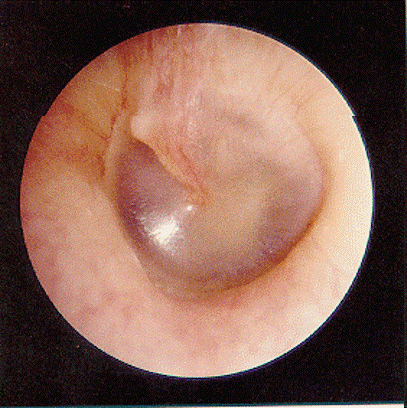
Internal Ear
External auditory canal is normal without inflammation; tympanic membrane is normal with a gray-white translucent appearance. No exudate or inflammation is noted.
Cranial Nerve Exam
- Cranial Nerves II thru XII were intact.
- Notably, CN VIII was intact. Normal hearing, no vestibular problems.
- CN V (trigeminal) was also intact, both motor and sensory. No mechanical allodynia noted in any of the 3 divisions of CN V. Possible masseteric hypertrophy.
Standard, Initial Pain Questions
There are some standard, initial questions to ask any patient with a chief complaint of pain:
- When did the pain first start?. Was anything related to its onset?
- What is the exact Location (point to all areas). Does it radiate to any other regions?
- Pain intensity (0-10) past week – now high low avg
- Is your pain constant, or on and off?
- Pain impact and interference on living (0 to 10).
- Pain aggravating factors?
- Pain alleviating factors?
- Effect of previous treatments?
- How would you describe your pain, e.g. Sharp or Dull?
- Any other pains or problems related to this pain?
Doctor Asks Maeve Initial Pain Questions

Maeve and her doctor sit across from each other.
The doctor asks, "Can you point right to the area of your pain?"
Maeve says, "Yes, it is right here but deep inside (points to her right auricular canal)."
"Do you feel pain anywhere else?" asks her doctor.
"No."
"Do you feel pain radiate anywhere else?"
"No," Maeve replies.
"How much pain are you experiencing right now, on a scale from 0 to 10, if 10 is the worst imaginable pain, and 0 is no pain?"
Maeves says, "6."
"What was it at its worst this past week?"
"7," says Maeve.
"What was the lowest your pain has been?"
"2," replies Maeve.
"What was your average pain intensity over the past week?"
"4 out of 10."
"Is your pain present all the time, or does it come and go?"
"Now it is constant. It started out with pain just now and then, but now it is there all the time."
The doctor says, "That must make it difficult to carry on other activities."
"It does," Maeve replies.
"How much does this ear pain interfere with your daily activities, if zero meant no interference at all, and 10 meant you were unable to carry on any activities?"
"Well, that’s a hard question to answer since it varies."
"What would be your best guess as an average for the past week?"
Maeve says, "I would say a 5."
"What activities are limited now? What can’t you do now that you could do before?"
"I don’t feel like being around other people as much, and it can be difficult to talk sometimes."
"OK, because jaw movement like talking is painful now or because conversing is difficult in general with people?"
Maeve says, "Well, I would say both."
"That sounds difficult to live with. I am sorry," the doctor commiserates. "Is it ok to ask you some additional questions so I can get a better handle on your problem before I take a look at this area?"
"Yes," says Maeve.
"What have been factors that aggravate or make your pain worse?"
"Stress, talking a lot," says Maeve.
"Anything else?" the doctor asks.
"Well I think it is worse in the early morning, then it can get better, but then get worse again in the evening."
"What are some factors that decrease your pain?"
"It seems like Advil can help a little. Also if I have hot showers, have a quiet weekend away from stress."
"How many Advil did you take each day?" asks the doctor.
"I took 2 at a time, for a total of 4 one day."
"How much did your pain reduce?"
Maeve says, "By about half, I would say, sometimes less when I only took 2 pills."
"Have any other medications seemed to help reduce your pain?"
"No I have not tried any others."
Summary of Maeve's Answers to Initial Pain Questions
When did the pain first start?
2 months ago.
Was anything related to its onset?
Stressors related to money, unemployment.
What is the exact Location (point to all areas)?
Deep Right Ear.
Does it radiate to any other regions?
YES – temple, forehead, face, neck.
Pain intensity (0-10) past week
Now (6), high (7), low (2), avg (4).
Is your pain constant, or on and off?
Became constant last week.
Pain impact and interference on living (0 to 10).
5/10 – difficulty talking, being around others since pain is distracting.
Pain aggravating factors?
Stress, talking a lot.
Pain alleviating factors?
Ibuprofen 400 mg reduces by half.
Effect of previous treatments?
Hot showers reduces by half.
How would you describe your pain, e.g. Sharp or Dull?
Maeve indicates both.
Any other pains or problems related to this pain?
No
Pain Locations Indicated During History
Ear
Maeve indicates the portion of her ear that causes her pain.

Temple
Maeve says her temple hurts and motions to her forehead during the history of her pain.

Jaw
Maeve motions to her face when she says her jaw hurts.

Summary of Maeve's Pain Condition So Far
- Likely acute pain – short duration, localized, responds to NSAIDS, moist heat.
- Acute Pain is progressively getting worse.
- Problem is in the region of the ear, but the temple neck and jaw muscles may also be affected.
- Aggravating factors are related to jaw function.
- Impact of pain is significant. Social isolation is a curious impact of the pain, and may indicate related psychosocial distress.
Other Methods to Discover Pain Location
Give patient standard picture of body – guide patient - have them sketch areas with pain – “Do you have any other pain in your body, such as…”
Pain Drawing
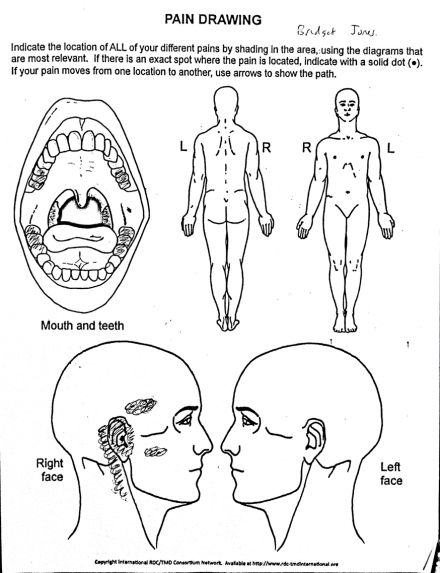
Maeve's pain drawing shows:
- Main complaint of pain in right auricular canal
- Pain only in orofacial region
- No other body sites show pain –– shows pain is relatively localized – think of underlying dermatomes of neural innervation.
Pain in Muscle Regions
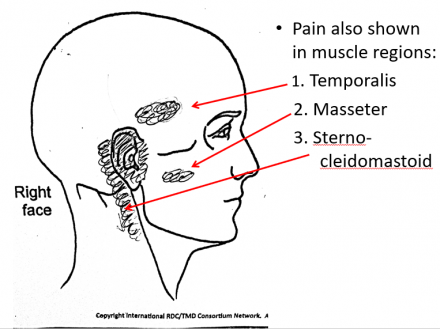
Maeve indicates pain in the following muscle regions:
- Temporalis
- Masseter
- Sterno- cleidomastoid
Pain in Mouth
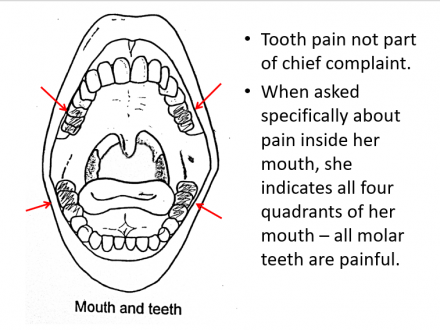
Maeve indicates the following for mouth and teeth pain:
- Tooth pain not part of chief complaint.
- When asked specifically about pain inside her mouth, she indicates all four quadrants of her mouth – all molar teeth are painful.
Primary Otalgia Versus Secondary Otaligia
Specific questions would you ask our patient to help differentiate between the main causes of otalgia (ear pain):
- Do you have any fluid or discharge from your ears?
- Do you have any ringing in your ears?
- Any dizziness?
- Does it seem like you have any loss of hearing? Can you hear just as well as before 2 months ago?
- Does your ear pain get worse with eating? Talking? Any type of jaw movement?
- Do any of your teeth hurt with hot or cold or with chewing?
Doctor Interviews Maeve to Determine Main Cause of Otalgia
The doctor says, "Now I would like to ask some specific questions about your ear pain."
"Ok."
"Have you noticed any fluid or discharge coming from your ear?"
"No."
"Any ringing in your ears?"
Maeve says, I" have some ringing in my right ear that is new. It seems to go up when I am stressed."
"Any dizziness?"
"No."
"Any problems with hearing out of your ears? Can you hear just as well as before 2 months ago?"
"No."
"You said your ear pain was worse with eating. Does it matter if the food is soft or chewy?" the doctor asks.
Maeve replies, "I can’t eat chewy foods anymore."
"Is that because the ear pain is worse?"
"Yes, definitely."
"Do any of your teeth hurt with hot or cold liquids?"
"Yes, on my lower back teeth on the left."
The doctor asks, "How long does it hurt?"
"Just for a few seconds, then it goes away," Maeve says.
"Any recent sore throat, colds or flu?
"No."
"Any pain with neck movement?"
"No, not really."
"Have you noticed any other problems related to your ears or close to your ears?" the doctor inquires.
"I don’t think so," Maeve says.
Summary of Maeve's Answers to Determine Cause of Otalgia
Do you have any fluid or discharge from your ears?
No.
Do you have any ringing in your ears?
YES, related to jaw function.
Any dizziness?
No.
Does it seem like you have any loss of hearing?
No change.
Can you hear just as well as before 2 months ago?
Yes.
Does your ear pain get worse with eating?
Yes.
Does your ear pain get worse with talking?
Yes
Does your ear pain get worse with any type of jaw movement?
Most.
Do any of your teeth hurt with hot or cold or with chewing?
Yes, all posterior teeth, for a few seconds.
EHR: History of Present Illness – Ear Pain
HPI: Ear pain focused questions:
- Patient denies fluid in ear, discharge, dizziness, hearing loss.
- Patient reports pain with eating chewy foods, transient tooth pain in all posterior teeth with cold, new onset tinnitus in right ear that varies in intensity with jaw function.
Temporomandibular Disorder Exam
Mandibular Range of Motion
95% females greater than 30 mm, 95% males greater than 35 mm.
Maeve has 32 mm opening (low normal) without pain 53 mm with pain in right TMJ region and R ear.
Right-Sided Structures Painful to Standardized 1 KG Palpation Force
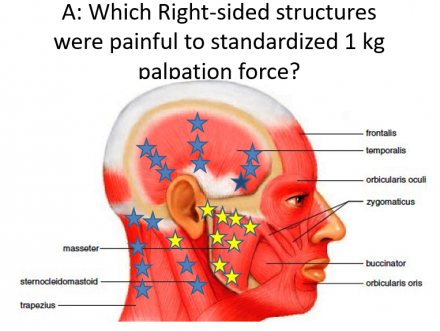
Head and Neck, Temporomandibular Exam Region Palpation Results
- Left side of head, neck and jaw – no pain
- Left TMJ – click (disc displacement with reduction)
- Right side SCM– Mild pain
- Superior Masseter- moderate pain
- Middle Masseter- moderate pain
- Inferior Masseter – moderate Pain
- Right lateral aspect of TMJ - Severe Pain
Intraoral Inspection, Dental Percussion Results
- Systematic inspection of upper/lower lips, labial mucosa, buccal mucosa, hard and soft palate, dorsum, lateral and ventral tongue, floor of mouth, tonsillar pillars and posterior pharyngeal wall all normal.
- Inspection with mirror and light show no obvious dental caries, periodontal pathology.
- Percussion of all teeth show that all molar teeth in all 4 quadrants of the mouth are slightly painful to percussion.

