The efficacy of analgesics and non-pharmacologic interventions are evaluated based on comparisons of sample norms, but there is tremendous variability in patients’ treatment responses.
Multimodal analgesia is a method of optimizing pain relief by targeting multiple sites of the nociceptive pathway. The multimodal approach relies on the rational use of medications and non-pharmacologic therapies (biobehavioral) with complementary mechanisms of action. This allows for use of lower doses of analgesics to potentially achieve greater pain relief and fewer adverse effects than could be achieved with single drug therapy.
Your patient reports jaw clicking with and without pain, and frequent headaches for 3 months. Treatments tried include acetaminophen, ibuprofen and oxycodone.
What is the mechanism of action for the different analgesics tried?
How does the mechanism relate to how pain is experienced? (choose the Neurology visit for more information)
Can genetics explain the differences in analgesic efficacy? (choose the Genetics visit for more information)
During this visit, the mechanism of action for analgesics will be outlined for a better understanding of their potential effectiveness for reducing or relieving your patient’s pain.
Neurochemical Mediators of Pain Pathway
Pain processing is modulated by neurotransmitters which are released from cellular or tissue damage and from the sensory terminals of presynaptic neurons.
To counteract pain input, activation of descending pain suppression pathways reduces the perceived intensity of pain or perception that the stimulus is painful.

Excitatory Mediators
Peripheral nociceptive afferent activity can be augmented if tissue damage has occurred due to release of pro-inflammatory factors such as prostaglandin E2 and bradykinins. Prostaglandins and bradykinins sensitize nociceptors to activation by low intensity stimuli.
Histamine and serotonin cause pain when directly applied to nerve endings.
Inhibitory Mediators
The monoaminergic neurotransmitters may also have pronociceptive effect depending on the subtype and location of receptors involved. Norepinephrine, serotonin, and dopamine modulate pain signaling in the dorsal horn and spinal trigeminal nucleus .
Endogenous opioids are key mediators in the descending inhibitory pathways and can inhibit pain signal transmission.
GABA is an inhibitory neurotransmitter that may also inhibit pain signaling.
Mechanism of Action of Analgesics
Analgesics reduce or relieve pain by a variety of mechanisms of action at a variety of different points on the nociceptive pathway. They can:
- Reduce the production of inflammatory mediators (e.g., nonsteroidal anti-inflammatory drugs (NSAIDs))
- Inhibit afferent nociceptive impulse transmission (e.g., opioids)
- Activate descending pain suppression pathways (e.g., opioids, anticonvulsants, monoamine re-uptake inhibitors)
- Suppress descending facilitatory pain pathways (e.g., opioids)
- Inhibit the release of excitatory neurotransmitter by pre-synaptic neurons (e.g., anticonvulsants)
- Inhibit nociceptive signal conduction by blocking of neuronal membrane sodium channels within tissues (e.g., lidocaine)
Prostaglandins
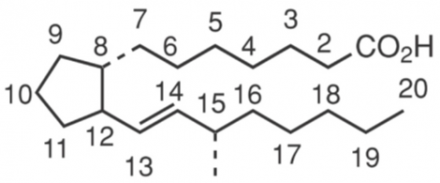
- Naturally occurring, 20-carbon cyclopentano-fatty acid derivatives produced from polyunsaturated fatty acids
- Derived from membrane phospholipids and unsaturated fatty acids
- Include prostaglandins, thromboxanes, prostacyclin and leukotienes
- Found in essentially every compartment in the body
- All naturally occurring prostaglandins have this substitution pattern
- 15α-hydroxy group
- Trans double bond at C-13
- αchain (carboxyl-bearing) and βchain (hydroxyl bearing)
- Classified by capital letters A, B, C, etc. based on nature and stereochemistry of oxygen substituents at 9- and 11-positions
- Number of double bonds in side chains designated by subscripts
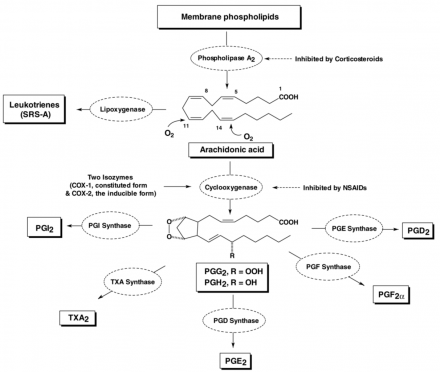
Mechanism of Action of Anti-inflammatory Drugs
Your patient tried two over-the-counter analgesics, Acetaminophen and Ibuprofen, a Non-Steroidal Anti-Inflammatory Drug (NSAID). Both NSAIDs and Acetaminophen are analgesics and antipyretics, but Acetaminophen is not considered an NSAID because it has little anti-inflammatory activity.
Acetaminophen inhibits prostaglandin synthesis in the central nervous system. NSAIDs also inhibit prostaglandin production by blocking cyclooxygenase both peripherally and centrally.
Anti-inflammatory drugs Interfere with:
- Immunological mechanisms (e.g., antibody production or antigen-antibody complexation)
- Activation of complement (excessive complement activation promotes local inflammation and is detrimental).
- Cellular activities such as phagocytosis
- Interference with formation and release of chemical mediators of inflammation
- Stabilization of lysosomal membranes
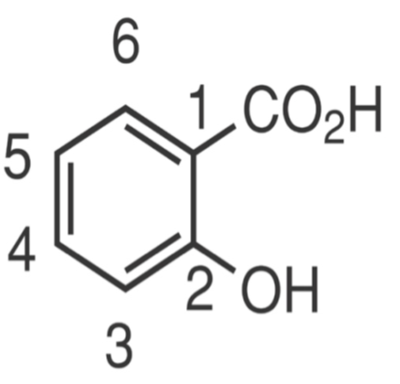
Aspirin
Hippocrates described chewing willow bark for pain relief in the fifth century! In 1838, Salicylic acid was obtained from salicin in willow bark and poplar bark.
Salicylate NSAIDs are classified as:
- Acetylated salicylate = aspirin, used medicinally in 1899
- The addition of the acetyl group causes irreversible inhibition of cyclooxygenase enzyme
- This also affects platelet aggregation by inhibiting formation of platelet aggregating factor thromboxane A2 for the life of the platelet
- Non-acetylated salicylates: choline magnesium trisalicylate
- Does not have an effect on platelet aggregation
Acetaminophen
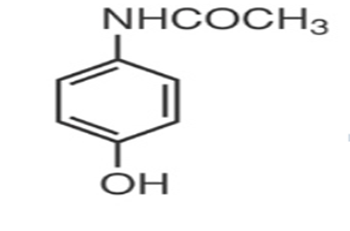
Acetaminophen has analgesic and antipyretic effects similar to aspirin, but limited anti-inflammatory effects.
Acetaminophen’s analgesic mechanism of action:
- Inhibits COX enzyme in the central nervous system (CNS)
- Possibly act on serotonergic inhibitory descending pathway and endogenous opioid pathway
Adverse effects are rare at therapeutic doses, and there are no major, clinically significant drug interactions with acetaminophen.
Acetaminophen is valuable for patients in whom NSAIDs are contraindicated because of side effects such as peptic ulcer, renal dysfunction, bleeding risks, and aspirin hypersensitivity.
View a diagram of PGH2 Synthesis
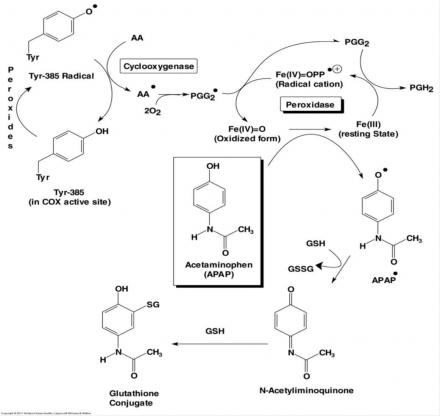
There are at least 20 different NSAIDs from six major chemical classes in the U.S., which:
- possess analgesic, antipyretic, and anti-inflammatory effects
- provide analgesia by reducing activation and sensitization of peripheral pain receptors are more effective than opioids for inflammatory or bone pain
There is a maximum dose limit. The dose, drug interactions, and side effects are not the same for all NSAIDs. The decision of which NSAIDs to choose varies among patients, and is based on side effects, convenience, and cost.
Most NSAIDs act as nonselective inhibitors of the enzyme cyclooxygenase (COX), inhibiting both the cyclooxygenase-1 (COX-1) and cyclooxygenase-2 (COX-2) isoenzymes. COX catalyzes the formation of prostaglandins and thromboxane from arachidonic acid.
The primary effect of NSAIDs is to inhibit the cyclooxygenase (COX) enzyme, which ultimately inhibits transformation of arachidonic acid to:
- Prostaglandins
- Prostacyclins
- Thromboxanes
However, many aspects of the mechanism of action of NSAIDs remain unexplained.
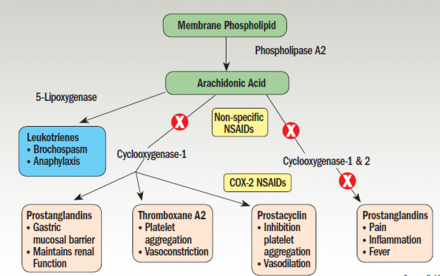
*Image: Pham T. Drug Topics. 2013;157(5):42-54
Cyclooxygenase (COX)
The extent of COX enzyme inhibition varies among the different NSAIDs, and there are no studies correlating the degree of COX inhibition with anti-inflammatory efficacy.
There are three COX isoforms identified:
- COX -1, “housekeeping” constitutive isoenzyme found in most tissues, which regulates gastric cytoprotection, vascular homeostasis, platelet aggregation, and kidney function
- COX-2, also known as Prostaglandin-endoperoxide synthase 2 (PTGS2)
- Undetectable in most tissues; constitutively expressed in bone, kidney, bone, female reproductive system
- Unexpressed under normal conditions in most cells, but expression increased during inflammation
- Expression of PTGS2 (COX-2) is upregulated in many cancers.
- COX-3 (relevance still unclear)
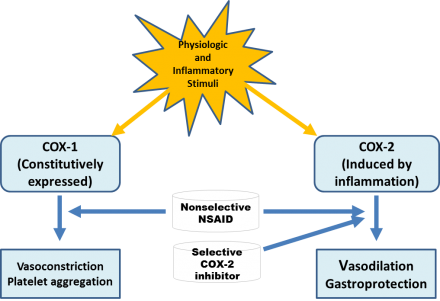
NSAIDs have different selectivity for the COX enzymes. This diagram indicates how selective each NSAID is for COX-1 or COX-2 inhibition.
It is the inhibition of COX-2 that produces the desirable effects of NSAIDs.
Celecoxib is the only NSAID available in the United States selective for the COX-2 enzyme. This is a major benefit for pain management of certain patients.
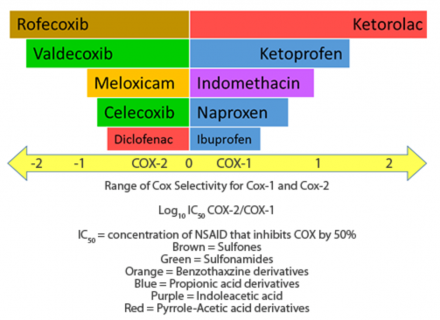
NSAID Selectivity for COX-1 and Cox-2 Enzyme
Patients with gastrointestinal (GI) complications, such as peptic ulcer disease (PUD), gastroesophageal reflux (GERD), and GI bleeding, may benefit from celecoxib. However, the COX-2 selective inhibition can increase the risk of cardiovascular (CV) events in patients with preexisting CV disease.
Aspirin possesses irreversible COX-1 inhibition and this has been shown to be cardio protective, which is apparent with low-dose aspirin.
This graphic represents the selectivity of common NSAIDs for COX-1 and COX -2 enzymes.

Anti-Inflammatory Comparison
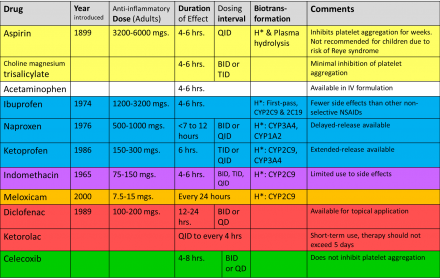
*Legend
mgs. = milligrams
hrs.= hours
H*= Hepatic
QD = daily, BID= twice a day, TID= three times a day, QID= four times a day
Yellow highlighted = Salicylates
Not highlighted = Acetaminophen, paraaminophenol
Blue highlighted = Propionic acid derivatives
Purple highlighted = Indoleacetic acid
Orange highlighted = Benzothaxzine derivatives
Red highlighted = Pyrrole-Acetic acid derivatives
Green highlighted = Cox-2 selective Sulfonamides
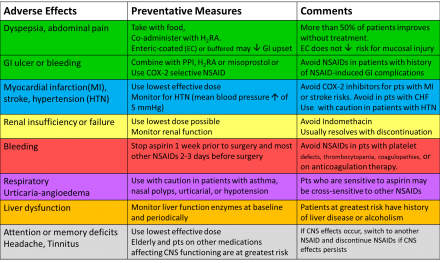
*Legend
Green highlighted = Gastrointestinal
Blue highlighted = Cardiovascular
Yellow highlighted = Renal
Red highlighted = Hematologic
Purple highlighted = Hypersensitivity
Orange highlighted = Hepatic
Gray highlighted = Central Nervous system
Test Your Knowledge
Question 1
Observable changes in vital signs must be relied upon to verify a child's or adolescent's statement that (s)he has severe pain.
Question 2
Because of an underdeveloped neurological system, children under 2 years of age have decreased pain sensitivity and limited memory of painful experiences.
Question 3
Children less than 8 years cannot reliably report pain intensity and therefore, the healthcare provider should rely on the parents' assessment of the child's pain intensity.
Question 4
Robert is 15 years old and this is his first day following third molar extraction. As you enter his room, he is lying quietly in bed and grimaces as he turns in bed. Your assessment reveals the following information:
- BP =120/80
- HR = 80
- R = 18
- On a scale of 0 to10 (0 = no pain/discomfort, 10 = worst pain/discomfort), he rates his pain as 8.
What number represents your assessment of Robert’s pain?
Question 5
In the case, the patient’s pain is well-localized, constant and described as throbbing. You suspect:
Question 6
Oral and Facial pain begins as a neural impulse (e.g., action potential) generated by peripheral neurons primary afferent neurons comprising this nerve of the temporomandibular joint?
Question 7
Higher level brain areas included in the descending pain modulatory system with a role in emotions and cognition, processing nociceptive information, and responsible for generating autonomic and neuroendocrine responses, include all listed below except:
Question 8
Ibuprofen and other non-steroidal anti-inflammatory agents are NOT effective analgesics for bone pain caused by metastases.
Question 9
Combining analgesics and non-drug therapies that work by different mechanisms (e.g., using acetaminophen, topical anesthetics, sucrose, and non-nutritive sucking) may result in better pain control with fewer side effects than using a single analgesic agent.
Question 10
The most likely explanation for why a child/adolescent with pain would request increased doses of pain medication is:

