Mildred along with her son Tommy visit Dr. Wright to seek help for her persistent knee pain.
Based on the history how intense would you rate Mildred’s pain?
- 1-4
- 5-6
- 7-10
- Do not know
Terminology and Scale
Use common terminology and an understandable scale.
Simply asking about pain may not provide an accurate assessment of the patients comfort. Many older adults deny pain due to the stigma surrounding it, but identify with other words such as ache, hurt, or discomfort. If you do not identify the word that the patient recognizes as their experience, providers may overlook significant pain and suffering. Older adults often have difficulty completing numerical pain scales (around 20 to 25%) such as the 0-10 scale. Older adults better identify with the verbal descriptor pain scale which uses words to describe pain severity. This scale is the most preferred by older adults and has the highest completion rate when compared to other pain assessment scales in persons with and without cognitive impairment. A modified verbal descriptor scale, the pain thermometer, is gaining in popularity and assigns a number to a corresponding descriptor in the backdrop of a thermometer. Taken together, key aspects of a pain assessment in older adults are identifying the pain terminology and scale that works best for the patient. Here are examples of the verbal descriptor scale on the left and the Iowa pain thermometer on the right. Remember, we need to find a pain severity scale that works best for the patient and continue to use the same scale on future visits to gauge the patient’s level of pain and the impact of our treatments.
Verbal Descriptor Scale
- Pain as bad as it can be
- Severe pain
- Moderate pain
- Mild pain
- No pain
Iowa Pain Thermometer
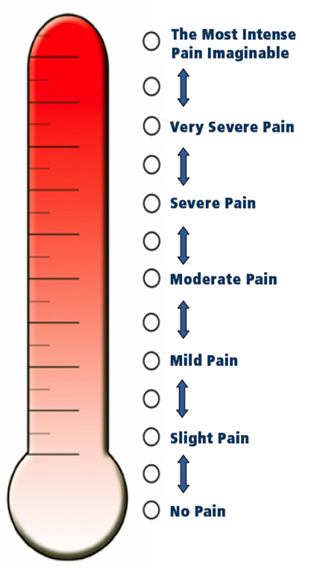
Reference
Herr K, Spratt KF, Garand L, Li L. Evaluation of the Iowa pain thermometer and other selected pain intensity scales in younger and older adult cohorts using controlled clinical pain: a preliminary study. Pain Medicine. 2007 Oct 1;8(7):585-600.
Cognitive Impairment
What clues occurred during the interview segment that indicate Mildred may have cognitive impairment? Can you mention any of them?
Additional Techniques
What additional techniques might you incorporate into your pain assessment to better understand Mildred’s pain experience?
Putting the Pieces Together
- Self-Report
- Pain terminology
- Verbal descriptor scale
- Potential Contributors
- Physical exam and history
- Pain including conditions, problems or procedures
- Caregiver Report
- Professional
- Non-professional
- Behavior Assessment
- Direct observation
- Screening or diagnosis
Fear of Pain in Patients with Dementia
Fear of pain can drive disability in older adults with dementia.
Pain can lead to fear of movement which can lead to sedentary behavior, before the cycle begins again.
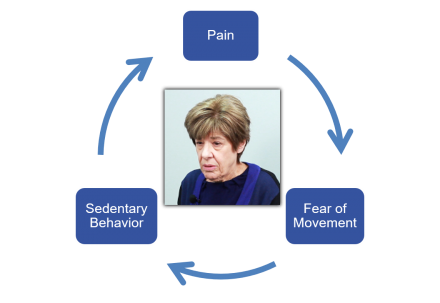
Another important consideration is to evaluate the extent to which fear of pain is impacting the ability of the older adult with dementia to function. A variety of stimuli may become increasingly unfamiliar as dementia progresses. So too may pain become more frightening, causing the patient to avoid movements associated with pain, and therefore, to become more sedentary and disabled. Thus a vicious cycle is created and evaluating and treating fear of pain becomes critical. Real-time evaluation of the patient can shed light on the extent to which fear needs to be treated. Consider, for example, the older adult with knee pain that reports inability to walk because of knee pain. Offer the patient your hand and walk along with them, or offer them a wheeled walker and observe their confidence in mobility. Improvement in walking performance as a result of providing external support offers a clue that fear may in part be driving pain behaviors. Such observations can help with both evaluating contributors to disability and in treatment prescribing.
Impaired Abilities Due to Chronic Pain
What abilities may be impaired in older adults when they experience chronic pain?
The Pain Signature
When patients experience pain, it may manifest in a variety of ways. We call this manifestation of pain as a patient’s pain signature. A pain signature may be particularly helpful to discern when patients with more advanced cognitive impairment are in pain. Pain can interfere with a range of functions including physical, psychological, physiological, and social. As part of a comprehensive pain history, providers should address the pain-related impact on each of these functions. This pattern of pain-related functional impairment represents the patient’s pain signature.
| Does pain affect your... | Not at all | A little | Somewhat | A lot | As much as I can imagine |
|---|---|---|---|---|---|
| Energy | X | ||||
| Mood | X | ||||
| Appetite | X | ||||
| Sleep | X | ||||
| Ability to do daily chores | X | ||||
| Ability to enjoy yourself | X | ||||
| Ability to think clearly | X |

