Misuse, Addiction, and Diversion: Prevention and Treatment
Addiction
Addiction is a complex phenomenon that has profound impacts on behavior and function.
The 5 ‘C’s of addiction:
- Chronic condition(there is a pattern of behavior)
- Cravings (withdrawal/dependence)
- Compulsive use (can’t stop thinking about using)
- Continued use despite negative consequences
- Control is lost (cannot stop using)
Diversion
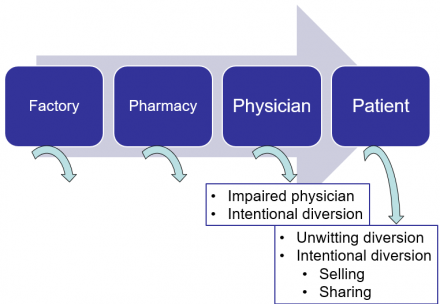
Misuse
- Patients misuse medications for a variety of reasons
- Inadequate understanding of proper use
- Under-utilization (side effects, fear of addiction)
- Over-utilization (failure to taper, excessive doses)
- Self-treatment of mood or sleep problems*
- Self-medication for uncontrolled pain (chemical coping)
- Uses medication to ‘get high’ (but not addicted)
- Addicted – uses to sustain habit
Prescription Drug abuse is a Major Societal Problem
These drugs were involved in 14,800 overdose deaths in 2008, more than cocaine and heroin combined.
The misuse and abuse of prescription painkillers was responsible for more than 475,000 emergency department visits in 2009, a number that nearly doubled in just five years.
More than 12 million people reported using prescription painkillers nonmedically in 2010, that is, using them without a prescription or for the feeling they cause.
Reference
https://www.pharmacy.ca.gov/licensees/rph_rx_painkiller_overdoses_policy_impact.pdf
Monitoring for Abuse, Addiction, Diversion
- Screen for risk of misuse prior to treatment
- Look for signs of withdrawal or unusual behaviors at clinic visits
- Monitor and document requests for early prescription refills: ‘my pills fell in the toilet’
- Counsel patients about safe storage, procedures for refills, monitoring practices: urine drug testing, opioid treatment contracts, ending treatment
- Contract patients for opioid treatment
Screening for Risk
Several screening tools exist:
Can use screening in the context of SBIRT:
- Screening, Brief Intervention, Referral for Treatment
Screening tools optmized for teens and adolescents include:
- CRAFFT (6 questions)
- DAST-A (28 questions)
- POSIT (139 questions)
Screening tools include:
- CAGE and AUDIT (alcohol)
- SOAPP (opioids for patients with pain
- (5, 14, and 24 question versions)
Potential resource: http://lib.adai.washington.edu/instruments/
Safe Prescribing
- Anticipate how much medication your patient will need for this specific problem:
- What dose is needed to control the pain
- How long will the pain last (days? weeks?)
- Write prescriptions on tamper resistant paper
- Check the prescription database in your state
- Contract with the patient:
- one prescriber
- one pharmacy
Treatment Contracts
Treatment contracts can provide for the following:
- Outline rights and responsibilities of patient
- Clarify rights and responsibilities of the provider
- Specify occurrences that violate the treatment contract
- Detail plans for monitoring treatment
- Provide for treatment cessation
Urine Drug Testing
- May be required
- May occur randomly or a specified intervals
- May indicate that a patient is taking or not taking the prescribed medication
- May indicate that patient is taking medications or substances that are not prescribed
- Are an important part of substance abuse treatment programs but may not be required for all patients with pain, depending on risk assessment
Realities
- Opioids are subject to abuse.
- At least 20% of patients do not use opioids as prescribed.
- Physicians are responsible for prescribing opioids safely and only as part of a comprehensive pain treatment plan.
Summary
- There are multiple ways in which pain relieving medications are subject to diversion, abuse, and misuse.
- Prescribers need to implement strategies to assess and mitigate the abuse of prescription pain relievers; this may include the use of screening instruments, urine drug testing and treatment contracts.
- Prototypes and validated instruments are available for safe drug prescribing.

