Tylee's Health History
- Social
- Lives with grandparents
- Attends college for fashion marketing 3 days/week
- Works part-time in a warehouse 2 days/week
- Health
- Treatment facility/hematologist remains the same as when he was a child
- Hospitalizations
- Cannot remember last hospital visit
- Medication
- Prevention of Sickle Cell Disease (SCD) Symptoms:
- Penicillin and folic acid
- Treatment of Sickle Cell Disease (SCD) Pain:
- Ibuprofen
- Then acetaminophen with codeine if needed
- IV morphine if needed (only in hospital)
- Prevention of Sickle Cell Disease (SCD) Symptoms:
- Self-Care Management
- Warm baths, showers, eats well, and gets plenty of rest
How Tylee Deals with Sickle Cell Disease Pain as a Young Adult
Advocacy
- Tylee must speak up and request the care he believes is necessary for his pain
- In order to receive proper pain management, Tylee must educate the interdisciplinary team about his sickle cell disease
20-Year-Old Tylee Advocates for His Health
Treatment
- Opioid analgesics titrated to pain relief with observation for side effecs
- NSAID: oral ibuprofen, intravenous ketorolac
- Stay hydrated
- Avoid infection (immunizations)
- Heat
- Massage
How Doctors Decide on a Proper Treatment for Tylee
Impact of Opioids
Opioid Use and Sickle Cell Disease (SCD)
- Some patients have described sickle cell disease related pain as "the worst pain one can suffer," worse than post-operative and cancer-related pain.
- This pain is the leading cause of emergency room visits and hospitalizations among sickle cell patients.
- Long-term therapy with opioids can be safe and effective and in selected patients, the benefits outweigh the risks.
- Reducing access to prescription opioids for sickle cell disease patients:
- Increases emergency room visits
- Stigmatizes Sickle Cell Disease (SCD) patients as engaging in drug-seeking behaviors
- Denies patients an effective way to manage their severe pain crisis
Reference
Opioid crisis adds to pain of sickle cell patients. Available at: https://www.nhlbi.nih.gov/news/2017/opioid-crisis-adds-pain-sickle-cell-patients Accessed May 15, 2019
Risks of Opioid Use
- Risks of opioid use and potential for abuse with sickle cell disease patients are relatively low
- Fear those diagnosed with Sickle Cell Disease (SCD) are more likely to become addicted to opioids, which means patients with SCD may be stigmatized as "drug-seeking."
- 63% of nurses believed patients with SCD were opioid abusers
- Clinicians assume opioid addiction is more likely in patients with SCD than other chronic pain syndromes
- Sickle Cell opioid deaths remain relatively consistent while those in the general population have increased, nearly quadrupling.
Reference
Ruta NS Ballas SK., 2016
Diagnosis
- Severe Sickle Cell Disease (SCD) Pain/Vaso-Occlusive Crisis (VOC) Pain
- Low back pain and headache
- Leg pain (bone pain)
- Chronic joint pain
New Strategies for Managing Vaso-Occlusive (VOC) Pain
Ketamine
- NMDA receptor antagonist with strong analgesic properties
- NMDA receptor effects may modulate central sensitization and hyperalgesia that are associate with recurrent Vaso-Occlusive (VOC) and therefore reduce opioid requirements
- Low dose infusion associated with lower pain scores and reduced opioid usage
- Trial of intranasal ketamine is underway
- Oral ketamine may also be effective
- Only given in the hospital (IV administered)
Reference
Hagedorn JM Monico EC., 2019; Manwani D Frenette PS., 2013; Young JR., et al., 2017; Jennings CA, Bobb Bt, Noreika DM Coyne PJ., 2013
Dexmedetomidine
- Dexmedetomidine: a specific α2-adrenoreceptor agonist with analgesic and mild sedative properties without respiratory depression
- Dexmedetomidine infusion associated with reduced pain scores, decreased opioid requirement in patients with pain unresponsive to escalating opioid dosage and ketamine
- Only given in the hospital (IV administered)
Reference
Hagedorn JM Monico EC., 2019; Manwani D Frenette PS., 2013; Young JR., et al., 2017; Jennings CA, Bobb Bt, Noreika DM Coyne PJ., 2013
Vaso-Occlusive Crisis Prevention Methods
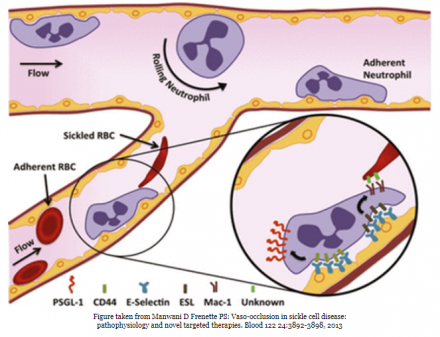
Crizanlizumab
- Monoclonal antibody that binds to P-selectin, blocking interaction with PSGL-1, decreasing leukocyte adhesion to vascular endothelium
- Administered monthly by infusion
- RCT 198 patients 16-65 yrs for 52 weeks
- 1.63 vs. 2.98 VOC per year
- No use in childhood yet
Reference
Atage KI, Kutlar A Kanter J., 2017
Glutamine
Reduces oxidative stress of sickled RBC
Decreases endothelial adhesion
RCT 230 patients 5-58 yrs in 2:1 ratio
25% reduction in crises over 48 weeks
Decreased ED visits and hospitalizations
FDA approved
Reference
Niihara Y, e al., 2018
Test Your Knowledge
Tylee is your patient. He is complaining of sickle cell pain in his legs and knees. Which non-pharmacologic approach would you recommend in combination with an appropriate analgesic based on his pain score?
Tylee's Discharge Plan
A follow-up appointment is arranged with the hematologist in 3-5 days unless symptoms worsen.

