
Diana is a 19 year-old woman with pelvic pain and jaw pain since adolescence.
You are meeting her for the first time.
She is seeing her provider for advice on how to manage her pain as it seems to be getting worse and is limiting the things she likes to do like dance and eat her favorite foods.
Interview with Diana
One way to start your interview is to encourage a personal pain narrative to allow Diana a few minutes to frame her story. This encourages her to share her pain story, can help you structure your assessment, allow her to feel heard, and aid you in responding empathically – and in the end will help with efficiency.
Diana's Pain Narrative
Pain Assessment Strategies
One way to organize your questions can include using the mnemonic “OPQRST”:
O – Onset: When did the pain start? What was happening at that time?
P – Palliative and Provocative factors: What makes the pain better? Worse? (Include specific activities, positions or treatments.)
Q – Quality: Describe the pain. Is it burning, sharp, shooting, aching, throbbing, etc.?
R – Region and Radiation: Where is the pain? Does it spread to other areas?
S – Severity: How bad is the pain? How does it affect your functioning and activities?
T – Timing: When does the pain occur? Is there a cycle to the pain?
Ensure that you also obtain a full medical history including other medical problems as well as a psychological, trauma, social, and current or past substance use history.
Diana's Pain Assessment
The Numeric Rating Scale
You may ask her to rate the severity of her pain on a scale from 0 = “No Pain” to 10 = “Worst Pain”. Although a numeric rating scale score can help to “quantify” someone’s pain, some limitations to using a numeric rating scale may include:
- Patients with chronic pain often report > 6/10 pain.
- A pain score may not reflect functional abilities.
- A number represents a static point in time (e.g. right now) which may be best for acute/procedural pain.
- A better way to evaluate chronic pain is to ask about the least, average, and worst pain intensity over time (e.g. past week or past month).
Pain Diagram
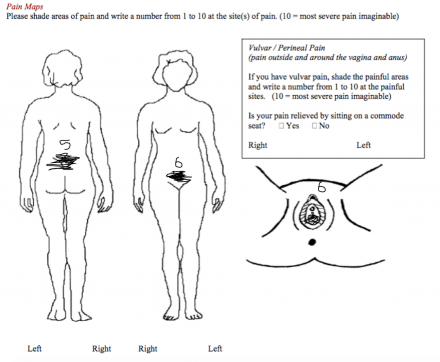
Reference
From the International Pelvic Pain Society Pelvic Pain Assessment Form 2008, www.pelvicpain.org
Pain Disability Index
- An objective measure to track pain’s effect on function is the Pain Disability Index
- This tool allows the provider to quantify the impact of pain on daily functioning, i.e. how much pain disrupts daily life
- This tool can be useful to track pain and disability over time as a way of measuring treatment effectiveness and Diana’s improvement
Reference
Pollard CA. Preliminary validity study of the pain disability index. Percept Mot Skills. 1984;59(3):974.
Pain Disability Index: Categories
7 categories rated from 0 (no disability) to 10 (worst disability):
- Family/home responsibilities (housework, errands, family duties, etc.)
- Recreation (hobbies, sports, leisure activities)
- Social activity (social functions with friends and acquaintances)
- Occupation (volunteer and/or paying jobs)
- Sexual behavior (frequency and quality of one’s sex life, or “0” if not sexually active for reasons other than pain (e.g. no partner))
- Self care (personal maintenance and independent living, e.g. bathing, etc.)
- Life-support activity (basics like eating, sleeping, and breathing)
Maximum score is 70 and can be tracked over time to evaluate treatment effectiveness, patient progress, etc.
Diana's Pain Disability Index
Diana scored the following (0= no disability, 10= worst disability):
- Family/home responsibilities: 2
- Recreation: 5
- Social activity: 3
- Occupation: 1
- Sexual behavior: 5
- Self care: 0
- Life-support activity: 0
Total score: 16 = mild impairment in function
Central Sensitization
You tell Diana:
- Pelvic and jaw pain can co-exist and go hand-in-hand with also other pain problems. Your history makes me think you may have endometriosis and a temporomandibular joint problem.
- These types of pain call also be impacted by “central sensitization.” There can be brain inputs that affect pain signaling and processing in addition to problems in the periphery such as in joints, peripheral nerves and muscles.
- Treating your pain will benefit from a multimodal approach targeting all of these areas to help improve your function.
- I will also have you see a dental colleague to help address the jaw pain.
- Helping you to feel better will take time but we will get there!
Introduction to Central Sensitization
This can be thought of as if the patient’s pain perception “volume control setting” is turned up too high. A patient without chronic pain would interpret the same pain signal at a lower “volume” setting.
Central Amplification
In central sensitization, the nervous system circuitry changes: there are increased pain transmission signals but decreased inhibitory inputs leading to an enhanced pain response.
Reference
Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain, 2011;152(3 suppl):S2-15.
Central Sensitization and Overlapping Pain Conditions
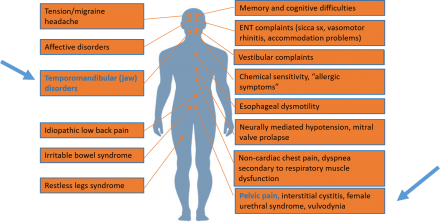
What is Endometriosis?
Definition and Facts
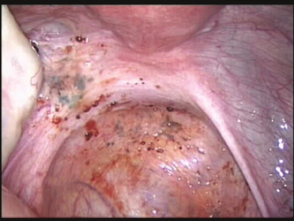
- Characterized by presence of endometrial tissue in sites outside of the uterus
- Common in reproductive-age women
- It is thought be an estrogen-dependent disorder
- Prevalence is up to 10% in the general population
- Up to 20% of women with endometriosis have another chronic pain problem such as irritable bowel syndrome, interstitial cystitis/painful bladder syndrome, fibromyalgia, and migraine headaches
- Infertility can be common
- Pain is the most common symptom:
- Dysmenorrhea (cyclical pain with menses);
- Dyspareunia (pain with sexual intercourse);
- Pelvic or abdominal pain;
- Referred pain in other sites may also be present (e.g. back pain)
Reference
Brown J, Farquhar C. Endometriosis: an overview of Cochrane Reviews. Cochrane Database Syst Rev 2014; (3):CD0099590.
How to Diagnose Endometriosis
- Endometriosis is often a “diagnosis of exclusion” and other diagnoses need to be ruled out, thus often unfortunately delaying diagnosis and treatment.
- Experienced providers can diagnose based on history and physical exam in 80% of cases.
- Imaging (MRI or ultrasound) may be of some help in diagnosis.
- There is insufficient data to support use of blood tests (serum markers) in diagnosis at this time.
- Trial of suppressive hormonal therapy can help with diagnosis (e.g. pain may improve if a patient is on continuous birth control and not menstruating).
- Gold standard currently remains laparoscopic surgery to visualize endometriosis lesions in the peritoneal cavity (which can be biopsied and/or removed).
Reference
- Hsu AL et al. Invasive and non-invasive methods for the diagnosis of endometriosis. Clin Obstet Gynecol 2010; 53(2): 413-419.
- Nisenblat V. et al. Blood biomarkers for the non-invasive diagnosis of endometriosis. Cochrane Database Syst Rev 2016;(5):CD012179.
How Endometriosis Causes Pain
- The ectopic tissue implants can bleed when activated during a menstrual cycle, causing inflammation which can also lead to scar tissue (adhesions).
- When pain is chronic, the central nervous system is also activated and involved and can lead to a perpetuation of pain signaling.
- In addition, chronic inflammation can lead to a patient suffering from referred pain to other muscle sites such as the lower back.
- Many women with endometriosis also have pain that originates from the pelvic floor musculature that cannot effectively coordinate contraction and relaxation. This is called pelvic floor dysfunction.
Symptoms Pelvic Floor Dysfunction Can Lead To
- Pain in the back, hips, sacroiliac joint
- Bladder emptying difficulties
- Vaginal and/or rectal pain
- Urinary frequency, burning or pain
- Constipation or diarrhea
- Painful bowel movements and fecal incontinence
- Painful intercourse
- Painful speculum and gynecologic exam
- Pain with tampons
See also www.endometriosis.org for patient resources.

