Acupuncture In Sickle Cell Disease: Introduction
Kevin V. Ergil, MA, DACM, LAc, Dipl. OM (NCCAOM)
Professor, Finger Lakes School of Acupuncture and Oriental Medicine of NYCC
Learning Objectives
At the conclusion of this segment the learner will be able to:
- Describe the historical and regional origins of acupuncture
- Explain how an acupuncturist would assess and characterize sickle cell disease
- Be familiar with tongue inspection and pulse palpation findings
- Discuss the concept of “blood stasis” and how it relates to Sharee’s presentation
- Discuss approaches to acupuncture treatment planning
- Describe the current evidence base relating to acupuncture and sickle cell disease
- Describe the specific risks and adverse events associated with acupuncture
Study Questions
- Why is SCD not within the traditional scope of Chinese medicine?
- List 3 elements of an acupuncture assessment.
- How good is the evidence that acupuncture can help with SCD?
- What are the common and rare adverse events associated with acupuncture?
- Using an evidence-based medicine perspective—evaluating best evidence, clinical experience and patient values and preferences— would you recommend an acupuncture referral for Sharee?
Where is Acupuncture in Use?
- Acupuncture is a clinical modality that is frequently offered to pain patients
- Acupuncture is included in Traditional Chinese Medicine (TCM) and Korean Traditional Oriental Medicine (KTOM). It is an integral part of health care not only in China and Korea, but in Japan, Vietnam and other regions of Asia.
- Since the 1970s, acupuncture has been a licensed profession in the United States. Physicians and other professionals may also practice acupuncture.
What is Acupuncture?
- Acupuncture treats pain through the insertion of specialized needles into regions of the body determined by traditional theory, bioscience-based anatomy and physiology, and clinical assessment
- Needles range from .4 to .12 mm in diameter and from 15mm to 150 mm in length
- Needles are typically left in place for 20 minutes or up to 45 minutes, depending on the treatment plan. They are often manipulated to create stimulation.
- Needle insertion and stimulation elicits both local and central responses and has been demonstrated to reduce pain
Additional Needle Insertion
Use of Acupuncture in Sickle Cell Disease
- Traditional Chinese Medicine has rarely been used to manage sickle cell disease (SCD), because SCD occurs among Africans and is virtually unknown in Asian populations. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1770296/
- However, with the globalization of acupuncture , acupuncturists outside of China have sometimes used acupuncture to treat SCD patients successfully during crisis episodes. An acupuncturist in Lagos, Nigeria wrote that when he treated a case of sickle-cell crisis
- "…the result was so effective, dramatic and encouraging that four other cases of genotype SS/SC were also treated."
https://www.ncbi.nlm.nih.gov/pubmed/?term=sodipo+1993+sickle+cell
Traditional Chinese Medicine (TCM) Assessment
- Diagnostic procedures used by acupuncturists include taking a patient history and conducting a physical examination.
- The physical examination includes distinctively traditional elements such as:
- pulse palpation
- abdominal palpation
- channel palpation
- inspection of tongue and skin
- This assessment process is traditionally known as the Four Examinations.
The Four Examinations
In Chinese medicine, the "4 Examinations" move from the least to the most intimate.
- Inspection
- Visual examination of any aspect of the body including the tongue, excreta and discharge.
- Listening and smelling
- Auditory and olfactory assessment of the character of sounds (vocalization, coughing etc…) and smells produced by the patient or their excreta and discharge.
- History taking
- This includes history of chief complaint, review of systems and other aspects of a conventional history.
- Palpation
- Palpation of the body and arterial pulses.
Taking the Patient's History
- When taking the history, a clinician is concerned with understanding the manifestation of pain, its location among body regions, and the triggers of vaso-occlusive crises (VOC) and other clinical complications.
- Sharee's subjective impression of "feeling cold" and her report that cold can trigger a crisis are diagnostically meaningful in understanding the condition, implicating both blood stasis and qi vacuity.
Significance of Tongue Inspection in Chinese Medicine
- The tongue is highly vascular and the status of its perfusion is readily apparent. Hence it can be used to assess the status of a patient’s circulatory system as a whole.
- The tongue tissue (body) and the overgrowth around the papilla (fur) are inspected. Erosion, scalloping of the tongue margins, sores, glossitis, and abnormal movement are useful signs in the tongue examination.
- The tongue is in close communication with the gastro-intestinal tract, so it can readily display GI changes and the status of the GI microbiome. Changes in the tongue fur indicate bacterial or yeast overgrowth.
Why the tongue is examined
Traditionally the tongue is:
- The "sprout of the heart"
- The heart, which governs blood, opens into the tongue
- External sign of the spleen (understood as an organ of digestion and blood production).
- "Root of the after heaven"
- The "after heaven" refer to physiological processes that commence after the first breath is taken and are the source of the generation of qi and blood
- Changes to the tongue body reflect the state of qi and blood of the viscera and bowels.
Inspection of the Tongue Body
- Color and sheen
- Pale and white suggest “cold” or insufficiency of blood
- Red and crimson suggest “heat” or inflammatory processes
- Congested purple shades suggest blood stasis (poor circulation)
- Form and bearing
- The shape and movement of the tongue can offer diagnostic insights
- Moisture
- Abnormal dryness or moistness can signal pathological processes
Normal Tongue Image
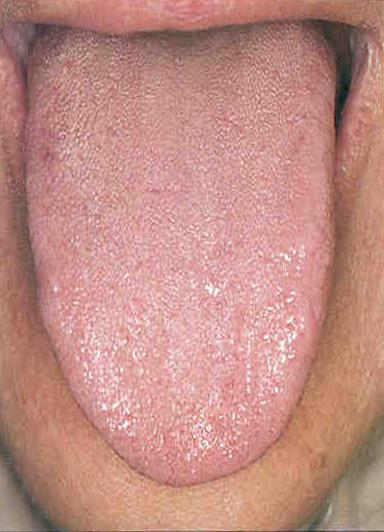
A normal tongue has a pale red (or pink) body with thin white fur (i.e., the tongue body to be readily seen through the fur)
- The tongue body should be
- Pale red, bright and moist
- Neither fat nor thin
- Supple, soft and flexible
- The fur should be
- Thin, white and evenly distributed
- Neither too wet nor too dry
Pale White or Red Tongue
Pale and white signify repletion cold
- Body is pale white, the fur is white, slippery and thick
- Yang vacuity that causes internal collection of cold damp is indicated by
- Body is pale white, the tongue body is enlarged and tender, damp and moist with much fluid, and on the sides of the tongue there are teeth impressions.
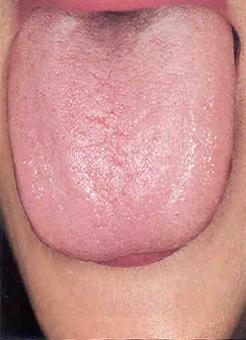
Kirschbaum, Barbara. 2010. Atlas of Chinese Tongue Diagnosis 2nd ed. used with kind permission of Eastland Press, Seattle.
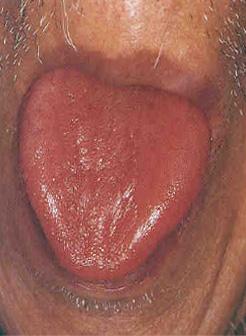
Red tongue
- Tongue color is deeper than normal
- Red governs heat
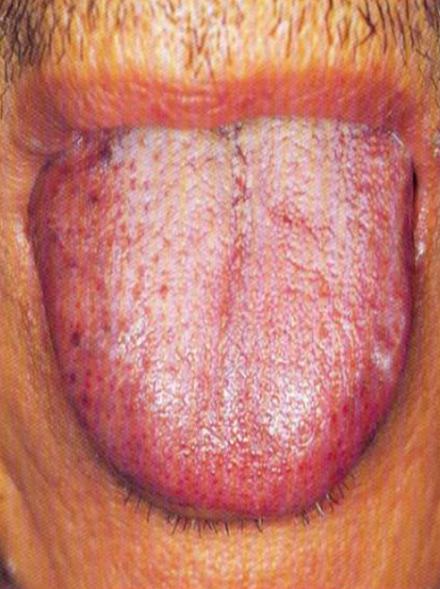
Tongue Fur
- Tongue "fur" is formed when papilla on the surface of the tongue trap debris such as bacteria and dead cells.
- Normal fur is so thin that the tongue body can be clearly seen.
- What aspects of the tongue fur are inspected?
- Development
- Color
- Thickness
- Moisture
- Traditionally, "normal" tongue fur is created from the rising and evaporation of stomach qi. It is a sign of healthy digestion and a functional microbiome.
- When disease develops, the fur thickens. This suggests a developing internal pathological process.
Inspection of the Tongue Form
Prickles are signs of heat and stasis
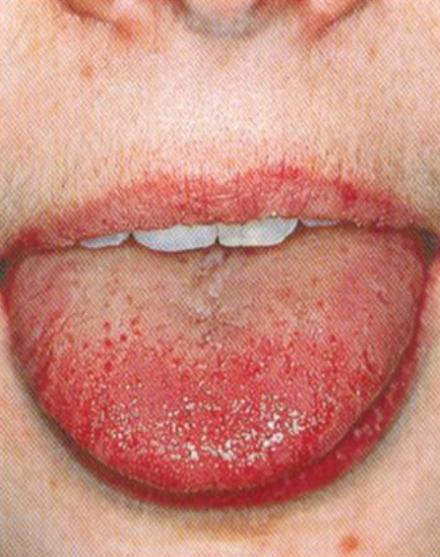
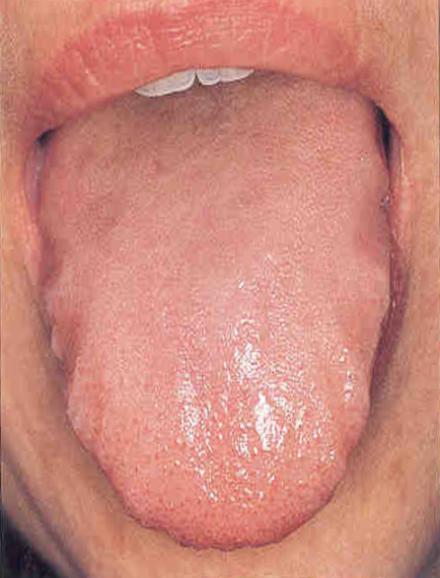
Teeth Impressions/Scallops are signs of qi vacuity and spleen vacuity
Pulse Diagnosis
Part of a palpation exam
- Used in conjunction with the findings of the 4 examinations (especially the history).
- Must be interpreted along with other information, such as how and when the condition arose, the nature of the patient's complaint, dietary irregularities, excesses of sleeping and waking.
Procedure
- One palpates the radial artery at the level of the styloid process of the radius, using the three middle fingers.
- Once the rate is assessed, varying degrees of pressure are used to determine the depth, force, rhythm, and quality of the pulse.
Traditional Perspectives on Pulse Diagnosis
- The heart and the pulse have a close relationship
- Heart governs blood and vessels
- Blood depends upon heart qi to move it around the body
- The pulse image can reflect physiological and pathological changes in the body.
- Heart qi is reflected in the rhythm of the pulse.
What Pulse Diagnosis Can Tell Us
- From the information provided by the pulse, various insights into the disease process can be obtained.
- Typically 28 standard pulse terms are used to describe commonly encountered pulse forms or 'images'. These terms characterize the pulse by
- Level
- Rate
- Force
- Rhythm
- Quality
Term #28. StringlikePulse /弦脉 xiánmài
- Clinically this is the most commonly seen pulse. Image/Description:
- Long and straight and stiff under the fingers
- Like touching the strings of a qin, think straight and long with energy and force
- Cause: Liver qi is not flowing smoothly/correctly, this can cause hyper tonicity of the channels and vessels, contraction of qi and blood or congestion of qi and blood.
Findings of Sharee’s physical examination
Pulse palpation and tongue inspection provide useful information relevant to Sharee’s case:
- Pulse palpation shows a "string-like" pulse, which suggests that liver qi is not flowing smoothly/correctly
- Tongue inspection shows thick white coating and heat speckles.
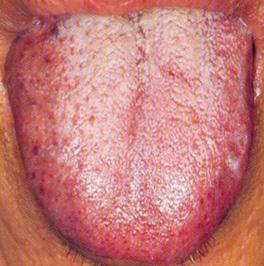
Assessment of Sharee’s Condition
- In traditional Chinese medicine, pattern diagnoses are identified by findings from the history and examination.
- Clinically, Sharee presents with pulse and tongue signs that are associated with the following specific diagnostic patterns:
- Qi Stagnation & Blood Stasis (impeded blood flow, vaso-occlusive crisis, acute chest syndrome)
- Qi and Blood Vacuity (fatigue and anemia)
- Dampness encumbering spleen and stomach (organ impacts of SCD, digestive disturbance)
Blood Stasis – Clinical Concept
- Blood Stasis was identified as a clinical entity in 200 BC, and over the centuries both traditional and contemporary scientific explorations of this concept have led to many clinical approaches to conditions characterized by poor perfusion or impediments to circulation.
- From a TCM perspective, blood stasis can both result from and contribute to pathological processes. In Sharee’s case, the signs of interior dampness as discussed in the video originate in blood stasis.
- Blood stasis is thought to be relevant to the treatment of many gynecological conditions, chronic hepatitis, scleroderma, multiple arthritis, Raynaud’s disease, and others.
Blood Stasis and Sickle Cell Disease
- The clinical presentation of SCD, because of its complexity and variable presentation, involves several diagnostic patterns. The characteristic pathophysiology of SCD, which is inhibited flow of blood, suggests the TCM diagnosis of blood stasis. The wide range of other systemic effects suggest other diagnoses as well.
- Blood stasis is general impairment of the smooth flow of blood, causing local stagnation of blood in the vessels or organs. Static blood and its resulting pathologies are characterized by fixed stabbing pain.
- In addition to her pain crises, Sharee has developed avascular necrosis or death of bone tissue due to lack of blood supply.
- She also has had symptoms of acute chest syndrome, which is a vaso-occlusive crisis of the pulmonary vasculature
Summary of Sharee’s Assessment
Specific TCM patterns are suggested by specific findings:
- Qi Stagnation & Blood Stasis
- Stress can produce onset
- Cold exacerbates or triggers
- Pain quality is similar to being cut and has a throbbing quality
- Qi & Blood Vacuity
- Hemolytic anemia can reduce RBC count
- Systemic impacts of SCD produce fatigue
- Chilliness can be a sign of qi vacuity
Choosing Points for Acupuncture Stimulation
- Effective acupuncture requires identification of precise acupuncture points for stimulation.
- The body is visualized to have a network of channels and vessels that connect a large number of acupuncture points
- The specific location of the patient\\\'s pain directs the choice of points for acupuncture stimulation.
- For example, the lung channel shown in the next slide connects a series of 9 acupuncture points that are potential targets for treatment of chest pain in a vaso-occlusive crisis.
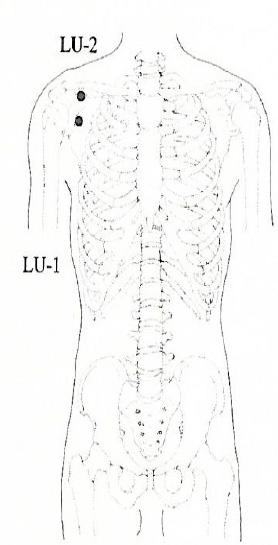
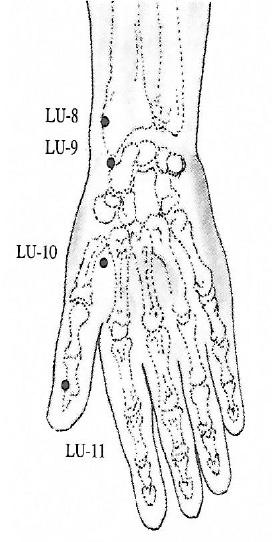
The Lung Channel
This figure displays the primary channel of the lung, as well as its connections to related channels and organs. The solid lines display the pathway on the shoulder and arm where points are distributed. The broken lines show how the channel is connected to internal organs. In Sharee’s case, channel points for acupuncture might be selected according to the regionalization of joint pain and, in cases of a vaso-occlusive crisis, of the pulmonary vasculature.
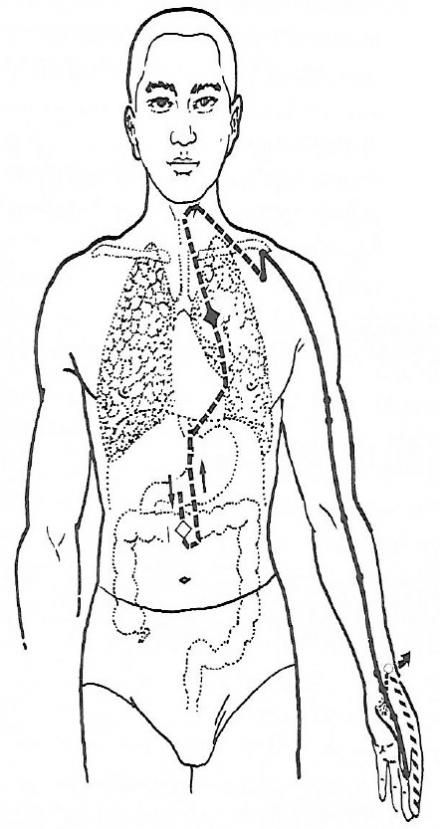
Other indicators of acupuncture points to target
- Tender Points
- Acupuncture points that are reactive on palpation may be particularly good candidates for treatment.
- Distal Points
- According to traditional theory, acupuncture stimulus is often applied locally and distally.
- For chest pain, points on the shoulder (LU-1) and the wrist (LU-9) are often targeted.
Planning Sharee’s Treatment with Acupuncture
- Acupuncture point selection is an important part of treatment planning
- In this case, points would be selected based on:
- Diagnostic patterns
- Regionalization of pain presentation (especially in vaso-occlusive crises)
- According to channel distribution
- Based on the tenderness of established acupuncture points
- Treatment would be revised, based on the patient’s response
Evidence for the Effectiveness of Acupuncture in Sickle Cell Pain
- The quality of the evidence base for the use of acupuncture in a range of painful conditions is steadily improving (Vickers et al. 2012, 2014, 2018 https://www.ncbi.nlm.nih.gov/pubmed/29198932)
- Evidence Map of Acupuncture (Hempel et al. 2014 https://www.hsrd.research.va.gov/publications/esp/acupuncture.pdf)
- The evidence base for the use of acupuncture in sickle cell disease is limited.
- The most robust and suggestive evidence is a retrospective study conducted at the National Institutes of Health from 2005 through 2011 examined outcomes 24 patients who received acupuncture (Lu et al. 2014 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4159140/)
- Pain outcomes for patients who received inpatient acupuncture for acute vaso-occlusive crises showed an average 2.1 point reduction on the 10 point numeric pain scale.
- The authors conclude that the findings suggest the possible use of acupuncture as an adjunctive method for managing pain in SCD.
- An early, small clinical trial (Co et al. 1979 https://www.ncbi.nlm.nih.gov/pubmed/523174) showed positive outcomes for acupuncture needling in VOC.
Acupuncture Adverse Events
- Minor risks
- Pain on needle insertion (commonly experienced)
- Bleeding, and bruising (commonly experienced)
- Transient nerve damage (relatively rare)
- Infection is typically rare when appropriate aseptic technique is used
- Sterile single use disposable needles, appropriate skin cleansing and handwashing substantially reduce risk.
- Organ puncture and damage to tissue
- Pneumothorax: comparatively rare, but possibly underreported
- Damage to heart, liver, kidney, spinal cord, spinal nerves, brain stem are rare.
Answers to Study Questions
1. Why is SCD not within the traditional scope of Chinese medicine?
- Sickle cell disease rarely occurs in Asian populations.
2. List key elements of an acupuncture assessment.
- Inspection (especially tongue)
- Listening and smelling
- History taking
- Palpation of the body (especially pulse)
These lead to determination of a pattern diagnosis
3. How good is the evidence that acupuncture can help with SCD?
- There is some evidence, but it is limited because TCM is not commonly practiced in countries with African populations. May be effective as an adjunctive therapy for chronic, poorly controlled pain.
4. What are the common and rare adverse events associated with acupuncture?
- Common:
- Pain on needle insertion
- Bleeding, and bruising
- Rare:
- Transient nerve damage (relatively rare)
- Infection
- Organ puncture and damage to tissue
5. Using an evidence based medicine perspective—evaluating best evidence, clinical experience and patient values and preferences—would you recommend an acupuncture referral for Sharee?
- Best Evidence: While the evidence for acupuncture specifically in SCD is limited, the evidence for acupuncture in managing some types of pain is very good. The limited data available on use of acupuncture in SCD suggests benefits.
- Clinical Experience: Clinical experience is limited because few SCD patients have access to acupuncture.
- Patient Values and Preferences: Sharee would like to have fewer episodes of vaso-occlusive crises and have a non-pharmacological method for reducing the severity of these painful episodes. The fact that opioids may induce or exacerbate acute chest syndrome should also be considered.
Resources
- American Academy of Medical Acupuncture. Conditions for which Medical Acupuncture May Be Indicated in a Hospital Setting. http://www.medicalacupuncture.org/ForPatients/GeneralInformation/HealthConditions.aspx. Downloaded 11/09/2015
- Ellis, Andrew, Nigel Wiseman, Ken Boss. Fundamentals of Chinese Acupuncture Revised Edition. Paradigm: Taos. 1991.
- Ergil M, Ergil K. Pocket Atlas of Chinese Medicine. Thieme: New York. 2009
- Hempel S, Taylor SL, Solloway M, Miake-Lye IM, Beroes JM, Shanman R, Booth MJ, Siroka AM, Shekelle PG. Evidence Map of Acupuncture. VAESP Project #05-226; 2013
- Kirschbaum, Barbara. Atlas of Chinese Tongue Diagnosis 2nd ed. Eastland Press:Seattle. 2010
References
- Co LL, Schmitz TH, Havdala H, Reyes A, & Westerman MP. (1979). Acupuncture: an evaluation in the painful crises of sickle cell anaemia. Pain, 7(2), 181–185.
- Lu K, Cheng M-CJ, Ge X, Berger A, Xu D, Kato GJ, & Minniti CP. (2014). A retrospective review of acupuncture use for the treatment of pain in sickle cell disease patients: descriptive analysis from a single institution. The Clinical Journal of Pain, 30(9), 825–830.
- Neeb, Gunter. Blood Stasis: China’s Classical Concept in Modern Medicine. Elsevier: St. Louis. 2007
- Sodipo J. (1993). Acupuncture and blood studies in sickle-cell anemia. The American Journal of Chinese Medicine, 21(1), 85–89.Sackett, David 2000 Evidence-based medicine: How to practice and teach EBM. Edinburgh.,
- Tsai S-L, McDaniel D, Taromina K, & Lee MT (2015). Acupuncture for Sickle Cell Pain Management in a Pediatric Emergency Department, Hematology Clinic, and Inpatient Unit. Medical Acupuncture, 27(6), 510–514.
- Vickers AJ, Cronin AM, Maschino AC, et al. Acupuncture for chronic pain: individual patient data meta-analysis. Archives of Internal Medicine. 2012;172(19):1444–1453.
- Vickers AJ, Linde K. Acupuncture for chronic pain. JAMA. 2014;311(9):955–956.
- Vickers, A. J., Vertosick, E. A., Lewith, G., MacPherson, H., Foster, N. E., Sherman, K. J., … Acupuncture Trialists’ Collaboration. (2018). Acupuncture for Chronic Pain: Update of an Individual Patient Data Meta-Analysis. The Journal of Pain: Official Journal of the American Pain Society, 19(5), 455–474.
- World Health Organization 2003 Acupuncture: Review and Analysis of Reports on Controlled Clinical Trials WHO, Geneva
- Xu XM, Zhou YQ, Luo GX, Liao C, Zhou M, Chen PY, Zhong M. (2004). The prevalence and spectrum of alpha and beta thalassaemia in Guangdong Province: implications for the future health burden and population screening. Journal of Clinical Pathology, 57(5), 517–522.

