Migraine Pathophysiology
Jennifer L. Mathews, PhD
Learning Outcomes
- List common migraine triggers
- Describe the pathophysiology associated with migraine
- Describe the role of serotonin and CGRP in migraine
- Describe the features of migraine with aura
- Describe migraine variants seen in children
What is migraine?
- A clear biological disorder
- Like asthma, diabetes, or hypertension
- A disorder of the central nervous system
- Hypersensitive to specific triggers and stimuli
- Often a family/genetic connection
- A disorder of nerve cells in the brain
- and the blood vessels surrounding the outside of the brain
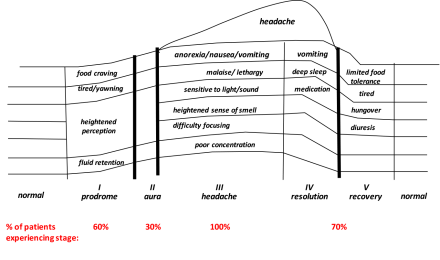
The five stages of migraine
What causes migraine
- There is NOT a single, clear, absolute answer
- Some ideas:
- Involves the trigeminal nerve and cranial arteries
- The nerves release CGRP (calcitonin gene-related peptide)
- Substance P and neurokinin A may also be involved
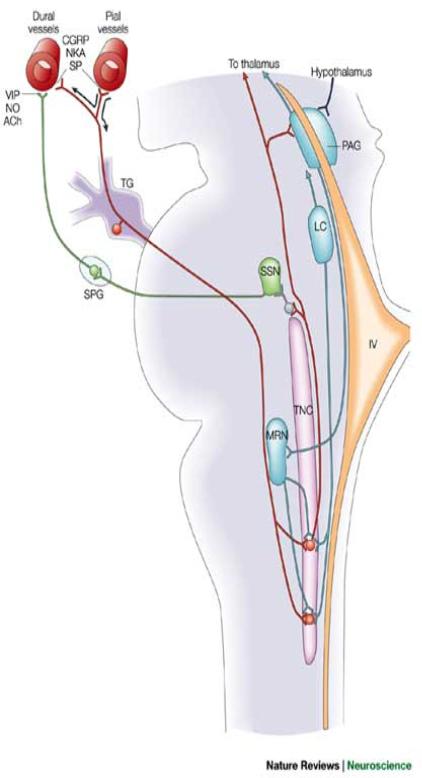
Trigeminal nerve system: pain in the brain
- Most of the brain does not register or transmit brain signals
- Trigeminal nerve system is responsible for transmitting pain signals
- Carries pain signals from meninges and blood vessels that surround the brain
- Pain is relayed through this network to the trigeminal nucleus in the brainstem
- From brainstem signal is sent through thalamus to the sensory cortex
Trigeminal nerves
- Convey pain via afferent C-fibers
- Sensory
- Terminations on cranial vessels, meninges, skin, and skull
- Also have projections to medulla and spinal cord
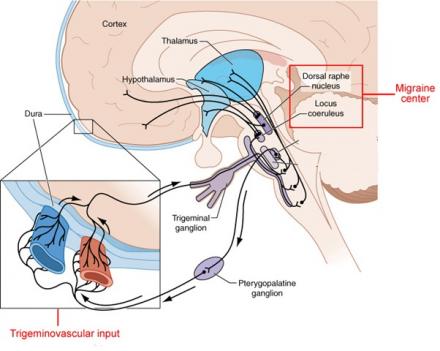
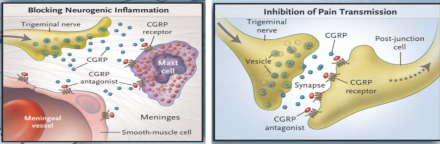
Image Source: http://pharmacologycorner.com/pharmacologic-treatment-migraine-pathophysiology-clinical-features/
What are common characteristics of afferent C fibers?
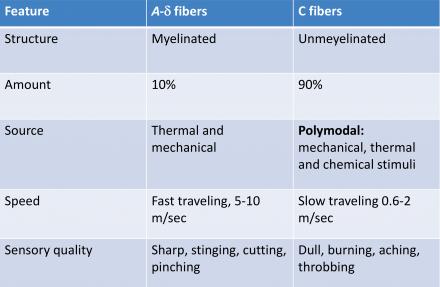
CGRP
- Calcitonin-gene related peptide
- Multiple reasons it may be involved in migraine:
- Potent vasodilator of cerebral and dural vessels
- Inflammation
- mast cell degranulation, fluid extravasation
- May alter pain thresholds
- Synthesized in trigeminal ganglion cell body
CGRP Elevation
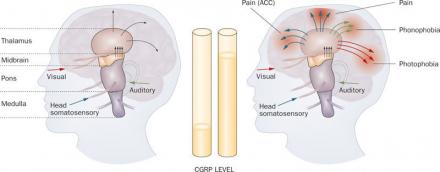
a | In the normal state, descending inhibition circuits, including those of the periaqueductal gray and locus coeruleus, process external sensory inputs to determine what information needs to be filtered, and what inputs need to be passed on to the thalamus and cortex. b | Various migraine triggers, such as stress, hunger or menstruation, could lead to elevation of the CGRP level and brain hypersensitivity. Sensory inputs that are normally filtered can activate various cortical regions, resulting in pain, photophobia and phonophobia. Abbreviations: ACC, anterior cingulate cortex; CGRP, calcitonin gene-related peptide.
Reference
http://www.nature.com/nrneurol/journal/v6/n10/fig_tab/nrneurol.2010.127_F1.html#close
Serotonin
- Role in migraine was believed to be associated with the "vascular nature" of migraine
- Causes vasoconstriction
- New theories re-examine this
- Focus on importance of modulating glutamate and CGRP
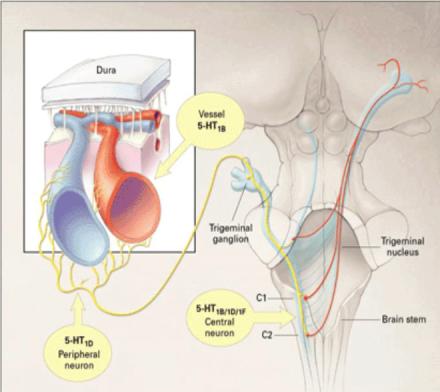
Serotonin and pain signaling
- Serotonin can inhibit calcium channels
- These channels are required for the release of glutamate and CGRP
- Serotonin inhibits:
- CGRP mediated inflammation/vasodilation
- Inhibits CGRP mediated sensitization
- Inhibits glutamate activation of NMDA channels, which are known to be involved in nociception
- Several types of glutamate receptors in the trigeminal nucleus (NMDA, AMPA, kainate, metabotropic)
The Migraine Cascade

Question: All patients experiencing migraine headaches have an aura.
Migraine with aura - visual
- Most common type of aura
- Is like an electrical or chemical wave that moves across the visual cortex of your brain
- As the wave spreads patient may experience visual hallucinations
- Visual auras are not the same for all people
- bright spots, flashes, hallucinations, loss of vision
- Commonly last 10 to 30 minutes

Image Source: http://migrainexpress.com/?tag=aura
Migraine with aura - sensory
- Can be with visual aura or on its own
- Often begins as a tingling in one limb or a feeling of numbness that travels up your arm over 10 to 20 minutes
- The sensation can spread to one side of your face and tongue
- Can causes transient speech or language problems
- dysphasic aura
In rare cases, the limbs and possibly the face on one side of your body might become weak
- hemiplegic migraine
Migraine with aura
- Aura usually precedes the migraine attack, but can also occur during
- An aura can also occur without an associated headache
- The migraine attack itself can last as little as four hours and as long as several days (typically 24-72 hr)
- The migraine is followed by a post-drome phase where the patient feels drained or washed out
- Some association with increased mortality from stroke and heart disease
- Counsel on lifestyle modifications
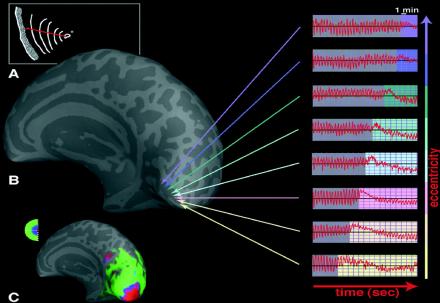
Role of Cortical Spreading Depression
- Evidence suggests that some migraine symptoms and auras are due to a phenomenon called cortical spreading depression (CSD)
- Begins with a wave of hyperexcitability
- As this neuronal activity progresses, the neurons eventually reach a state where they cannot fire anymore
- Channels become inactive
- This "depression" can be detected on MRI
- A decrease in regular brain activity in the occipital cortex has been correlated with patients' descriptions of migraine auras.
Cortical Spreading Depression
Who gets Migraines? Comorbidities
For many patients, migraine is associated with other illnesses such as:
- Depression
- Anxiety
- Stroke
- Irritable bowel syndrome
- Epilepsy
- Hypertension
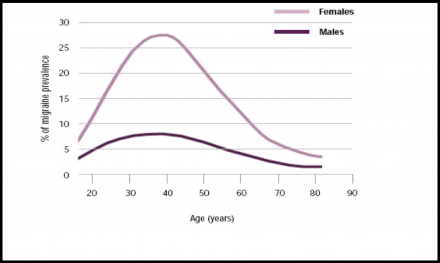
Women and Migraine
- Rate of migraine is approximately the same in children
- Change in rate at puberty
- One in four women has had a migraine
- Three times more women than men
- Hormones?
- Particularly estrogen, which fluctuates monthly
- Levels fall prior to menstruation
- If you are interested in learning more:
Migraines in Females vs. Males